Trends in Workers' Comp
Record Hospital M&A Deals Spell Trouble for Workers’ Comp Payers

Eliminating unnecessary emergency-room visits and other known cost containment measures is increasingly critical, with a record number of hospital mergers expected to squeeze workers’ compensation payers.
Health-system mergers set a record during 2017, with 115 announced deals. The trend continues in 2018, NCCI Holdings Inc. reported in a July 2018 Quarterly Economic Briefing.
Data shows that overall, the mergers increase hospital service prices 6 percent to 18 percent on average, NCCI said. Although such findings rely on health insurance and Medicare data, NCCI expects the mergers will accelerate the cost of caring for injured workers.
The current wave of consolidations began in 2010 and accelerated in 2014. It likely will increase both the quantity of care provided and the unit price of medical services, even in states attempting to control costs with workers’ comp hospital fee schedules.
“By combining former competitors in a market, consolidation has the potential to reduce competition, affect the quantity of care and increase prices,” the workers’ comp research and rating organization said. “Research to date on completed hospital mergers has yet to demonstrate the benefits of consolidation via improved quality, access and cost.”
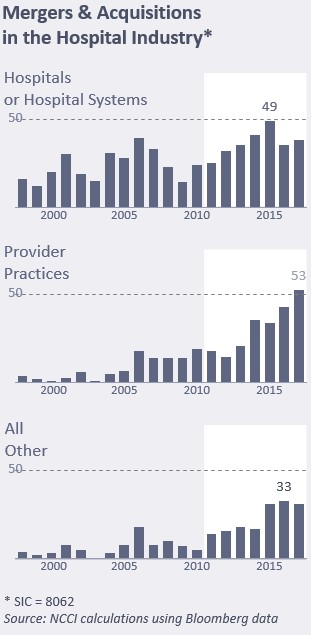 In addition to the mergers, hospitals acquired 5,000 physician practices between 2015 and 2016, driving a trend of more hospital-based doctors.
In addition to the mergers, hospitals acquired 5,000 physician practices between 2015 and 2016, driving a trend of more hospital-based doctors.
Health care consolidation reduces hospital operating costs by 15 percent to 30 percent, while improving care integration and eliminating clinical services duplication. But those reduced hospital operating expenses do not find their way to service price decreases, NCCI said.
A study on the precise impact of health care consolidation on workers’ comp does not yet exist, according to NCCI. That is why NCCI researchers referenced commercial insurance and Medicare data to report on the price and utilization increases accompanying health-system mergers.
“Even so, the trend toward increasing hospital consolidation is likely to have produced similar upward pressures on utilization and price in workers’ compensation as those observed for other types of health insurance,” NCCI reported.
NCCI plans to conduct further research into the impact of hospital services concentration on prices for workers’ comp medical care.
Renewed Focus on Cost Containment
The mergers make it increasingly obvious that employers and other workers’ comp payers must double down on strategies for eliminating unnecessary hospital visits and containing the cost of necessary visits.
The self-insured Southeastern Pennsylvania Transportation Authority’s practices for eliminating hospital expenses include training front-line supervisors.
The training educates supervisors on the benefits of addressing minor accidents, such as a bumped knee, with ice and perhaps a follow-up visit with a SEPTA network doctor rather than always considering an emergency room visit as the first line of treatment.
“That way you are not going through the most expensive portal for health care,’ said Rick Graham, SEPTA’s workers’ comp director.
The health system mergers and acquisitions will make proven measures for containing medical-provider expenses, such as bill-review systems and discounted provider network contracts, increasingly important, said Thomas Ryan, senior principal at Willis Towers Watson.
But history also shows that workers’ comp purchasers of medical provider networks will have less leverage when negotiating for the services when health-care provider options narrow.
For example, medical providers in rural areas, where there are fewer options for treating injured workers, historically negotiated for higher fees, Ryan elaborated.
Still, network discounts do have a history of reducing claims payer costs. But workers’ comp payers must make certain that prices are not the only consideration in the discounted health-provider contracts.
As hospital swallow up more health care services such as local clinics, workers’ comp network purchasers need to be certain the clinics and other services employ occupational-medicine doctors who are experts in treating the types of injuries employees typically suffer.
Clinics only dispensing family medical care won’t do, Ryan said.
Despite the cost and utilization challenges stemming from health-system mergers and acquisitions, there may be a bright spot.
Graham, SEPTA’s workers’ comp director, said his program benefits because the hospitals in his area have their own internal workers’ comp programs, such as return-to-work practices, for hospital employees.
Because of that, the doctors treating SEPTA employees now understand other employers’ return-to-work efforts and know they can safely release injured employees into a work environment prepared for their return.
As hospital swallow up more health care services such as local clinics, workers’ comp network purchasers need to be certain the clinics and other services employ occupational-medicine doctors who are experts in treating the types of injuries employees typically suffer.
Ryan, who has several hospital clients, said there is potential for SEPTA’s experience to become a more widespread trend.
As health systems merge, he is seeing hospitals pour resources into their own workers’ compensation risk management efforts. And, as hospitals acquire more doctor groups, the doctors working in hospital emergency rooms are now employees who may be learning more about their employers’ return-to-work programs.
In addition, with the doctors now employees rather than private-practice physicians who come and go, the newly employed doctors may have greater ability to learn about other local employers’ occupational health and return-to-work practices.
“They are no longer like the rent-a-docs that rotated through the emergency departments where there were a lot of irregularities as far as continuity of care,” Ryan said. “Now they are full-time employees familiar with different employers in the community.” &











