AI and the Adjuster: Driving Efficiency Without Losing the Human Touch

Artificial intelligence — bubble, bust, or beacon of change — is here to stay, including in the workers’ compensation industry. For claims professionals, the use of AI is more than an answer for heavy caseloads; it may help foster an increase in the adjuster’s ability to focus on the claims that need the most attention and allow for the enhancement of in-demand analytical skills.
However, as companies implement AI tools into legacy workflows, the question becomes where the industry can seek better efficiency and dependability while leveraging what only humans do best to drive better outcomes.
Predictive Models Lead the Way
Some AI tools have been used widely in workers’ comp claims management for at least the last several years; these primarily relate to the type of predictive analytics lauded by technology vendors as able to predict behavior or loss potential using statistics and proprietary data sets and algorithms.
“We have leaned heavily [into machine learning] for years. We use that in the form of predictive models and have used it for our adjusters to help them to make decisions at key points in the claim,” said Virna Alexander, EVP & chief claims officer at Liberty Mutual.
“Some of those models that we use give alerts for when a claim is likely to be severe or complex or where an early intervention would be helpful. We’ve used models to escalate when there’s specialized handling needed or where we think there might be fraud or the potential for loss recovery.”
Balancing Technology and Expertise
Growing existing capabilities with an eye toward enhanced administrative function is a common strategy among claims leaders, who remain rightfully concerned about reducing the presence of actual human expertise in claim processing, and ensuring they remain in compliance with regulatory requirements.
“We use AI to create efficiencies and return time to the field,” explained Ryan Murphy, vice president of product for enterprise claims at CorVel.
“The focus is not on replacing claim professionals, but on enhancing how they work. AI supports administrative workflows, helps identify claims that meet certain criteria, and surfaces opportunities that may require attention.”
Transforming Daily Claims Work
As AI tools become more pervasive and claims staff become more accustomed to using them, the effect has become marked for just about every process a claims manager employs to work their files day-to-day.
“It’s infiltrating every little bit of that process to give adjusters access to information they may not have had easy access to before,” said Steve Junker, chief innovation officer of accuro Solutions.
“Now, because they’re not having to give their mental energy to every hundred-dollar PT claim, they’re able to really dig into the complex claim of the guy who got his arm caught in the thresher. They can focus on the right treatment for that individual — that’s where their expertise will come to bear.”
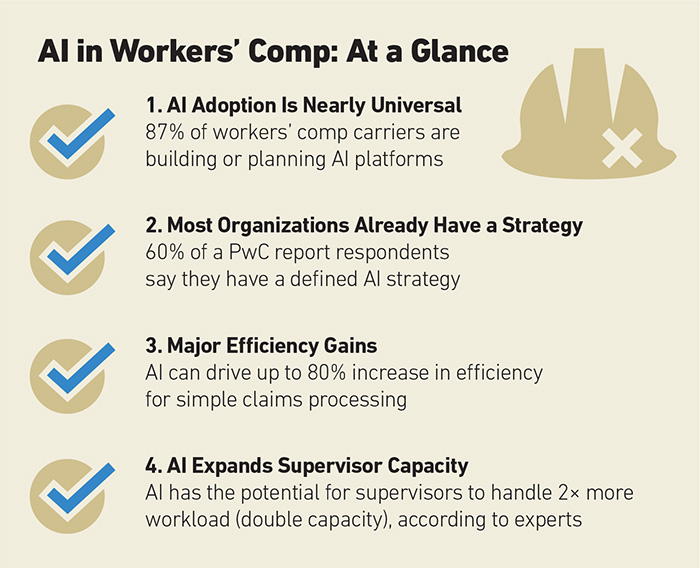
Importantly, this shift is inevitable. Not using AI in comp now is virtually unheard of: A recent PwC study found that 87% of its workers’ comp carrier respondents are building or are planning to build out their AI platforms.
This was combined with a finding that 60% already had a defined AI strategy. This is no surprise when preliminary findings suggest 80% increases in automated efficiencies for simple claims when AI is fully integrated into claims management.
“From a claims handling perspective, AI can be like a supervisor in a box on your desktop. You can load your best practices into the AI, which will have a pop-up and interactively work with the adjuster to go through the efficiency of that. Once AI is totally instilled, supervisors will have twice as much capacity,” said Ron Morrison, chief claims officer at MSIG USA.
Efficiency and Process Standardization
Operationally, this reduces mistakes, standardizes processes better than training could ever do, and frees up supervisors and claims adjusters to focus on the parts of the job that are more intricate, and more meaningful.
“Adjusters have more time and more capacity to handle more on a deeper level, which should create an expense reduction and drive better outcomes, at least theoretically,” Morrison offered.
“But I think the biggest thing that AI doesn’t bring and the biggest thing the industry lacks is negotiation skills. I think that’s where the focus is for my team.”
Indeed, the oft-cited adage that “20% of claims drive 80% of costs” may be a thing of the past if the majority of simple claims processing activities can be automated with the human adjuster simply checking in to make the final decision with the support of AI-assisted functionality.
However, as with any new technology, there are inherent risks, but experts say it’s important to understand these risks in context.
“When AI takes on repetitive, administrative work, such as reviewing or responding to emails, processing intake or referral document, or even authorizing routine requests aligned with medical guidelines, adjusters gain back time for what matters most,” said Mike Theis, AVP of product analytics & business strategy at Healthesystems.
“That time can be reinvested in understanding the injured worker’s situation, showing empathy, and building trust‑based relationships.”
“It’s not magic; it’s a tool. So, if we start with that mindset, it really helps us think about AI just like any other tool in the organization, ensuring proper oversight, governance, controls, as we’re building these systems and not after we build these systems,” said Prashant Hinge, chief information and transformation officer, MSIG USA.
“Yes, AI can help us do things good, fast, and cheap, which we’ve been trying to do for decades now, but the downside is that it can also do bad things very fast,” he added.
When it comes to doing bad things fast, the root of the problem is usually the data the AI is trained with — it’s the “garbage in, garbage out” principle of information technology taken to a new level.
“You really have to quantify where the data is coming from in the artificial intelligence pool and make sure that if you’re using vendors — are they using a captured data pool of our data or are they integrating and pooling data from other industry sources? My concern comes with vendors that are pulling data from public records or other services, and the integrity of that data,” said Morrison.
Keeping Humans in the Loop
Data sources and ensuring they’re the right fit for the AI solutions being used is essential, but the risk doesn’t end there.
“Even with robust data, it is essential to maintain a human-in-the-loop approach. Having experienced professionals review and validate AI-generated outputs helps ensure that subtle nuances and unique circumstances specific to each claim are appropriately considered,” said Rajeev Khanna, chief information officer at Trucordia.
“This collaborative workflow not only enhances the reliability of the analysis but also ensures that expert judgment is applied before any critical actions are taken, ultimately safeguarding both claim outcomes and organizational integrity.”
Despite this, the common refrain among claims leaders was that the benefits of AI outweigh the risks, and with the right operational posture, workers’ compensation stands to improve across the board with the adoption of AI tools, including with the younger generation of claims professionals entering the industry.
“There are a lot of workflows in our business that need to be automated. I think we’re going to be able to eliminate a lot of redundant, mundane tasks that people are having to perform,” said Cliff Belliveau, chief innovation officer, MyMatrixx.
“And if you look generationally, the farther you go toward Gen Z, and maybe Gen Alpha in a few years, younger folks have a lower tolerance for repetitive work/mundane tasks. AI’s going to be really helpful to personalize the customer experience better than we ever had before.”
Ultimately, stakeholders in workers’ comp, whether it’s the insured or the injured worker or the ecosystem of professionals and regulators that make the system run, will see AI transform an industry that depends on accurate and efficient communication.
“You’re going to type less to our customers and talk more to our customers — that’s what we need to do — type less, talk more. The more that big companies can do that, the better it gets,” said Hinge. &