Sponsored: Lexington Insurance
Managing Patient Safety in a New Health Care World
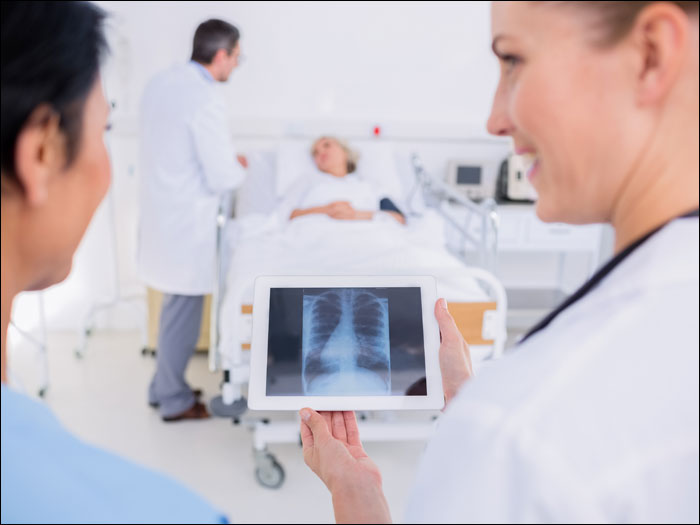
Much like regular screenings, exercise and a healthy diet, patient safety in health care institutions should be thought of as preventive medicine.
“Patient safety aims to relieve the burden of fixing mistakes by taking steps to prevent them from happening in the first place,” said Aileen Killen, head of casualty risk consulting, AIG.
With the right strategies and protocols in place, human error in delivering patient care can, to some degree, be factored out, mitigating the risk of things like falls or medication mistakes. And the outcomes-based reimbursement model enforced by the Affordable Care Act provides extra incentive to improve patients’ overall experience and reduce readmission rates.
Some challenges stand in the way, though, of achieving better safety.
For one thing, increased consolidation in the industry has brought risks associated with integrating disparate safety cultures and ensuring continuity of care if patients are moved to a new doctor. The trend of shifting more care out of main hospitals to ambulatory sites instead also creates concern that those outpatient facilities are not up to the same safety standards as larger organizations.
Finally, advancing technology — while offering great promise to eventually make health care more efficient and error-free — presents significant risks in its implementation while doctors, nurses and other health care professionals learn how to best use it.
Lexington Insurance, a member of AIG, is meeting the demand for more innovative tools to navigate the changing environment with a suite of safety assessment programs that identify problem areas and provide recommendations for improvement.
Assessing Safety Culture
 The first step in overcoming any challenge is assessing the situation in order to create the best strategy.
The first step in overcoming any challenge is assessing the situation in order to create the best strategy.
“Every health care organization should aim to become a ‘high reliability organization,’ or HRO,” said Brenda Osborne, division executive, health care, Lexington. “It’s a term borrowed from the airline and nuclear power industries, in which any employee has the right to shut down operations if they spot a safety issue.”
Lexington’s Best Practice Assessment tool allows organizations to compare their own protocols against evidence-based best practices and identify weak spots in their safety culture.
“We survey employees and ask if they feel free to speak up to people in authority,” Killen said. “If they can all say yes, you’re on the road to a safety culture. Then we drill down into specific high-risk areas.”
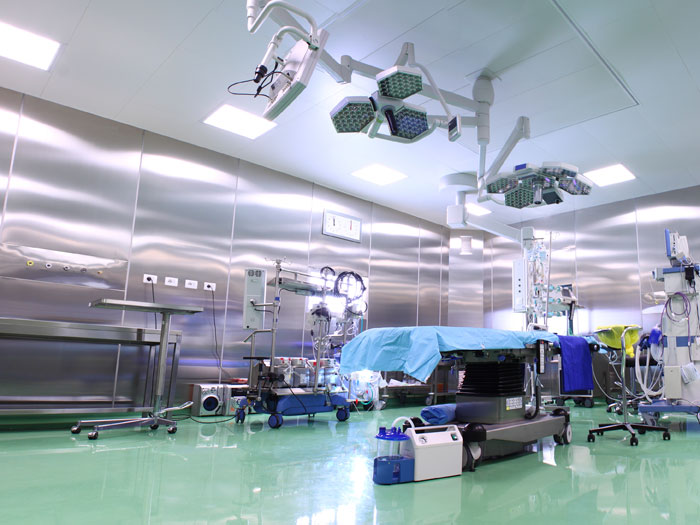
Clients can conduct specific assessments for error-prone areas like the emergency department, obstetrical department and operating room.
We give organizations recommendations on how they can improve in areas where they are deficient, and we can benchmark their performance against the best practice as well as against other institutions that have done the same assessment,” Killen said.
Those benchmark comparisons are key for securing leadership buy-in. Executives often need to see what other institutions are doing in order to feel confident in their decisions to make changes or invest more heavily in patient safety measures.
If another competitive hospital has better staffing ratios, for example, benchmark stats will show that and support the C-suite’s decision to hire more nurses to achieve a similar ratio.
“What it basically does is give the risk management, patient safety and quality improvement staff a roadmap for which areas to focus their activities for improving patient safety and risk management at their organization,” Killen said.
Acquisitions and Physician Employment
 The flurry of merger and acquisition activity in the health care industry creates new risks for large hospital networks that acquire physicians’ practices. The integration of different patient safety and risk management practices can prove difficult.
The flurry of merger and acquisition activity in the health care industry creates new risks for large hospital networks that acquire physicians’ practices. The integration of different patient safety and risk management practices can prove difficult.
“You have to take multiple approaches and mindsets and meld them into one fluid organization,” Osborne said. “That has a big impact on physicians’ ability to treat patients and deal with the appropriate hand-offs.”
“Patient hand-off is one of the biggest safety challenges,” Killen said. “Assigning a patient’s care to a different doctor leaves room for gaps in communication, which is so critical to making the correct diagnosis and keeping a medication schedule.”
Lexington’s Office Practice Assessment tool scores acquired practices on 14 different domains, including risk management and patient safety, communication, infection control and prevention, incident reporting and medication safety, among others. Recommendations are provided for any domain that scores less than a perfect 100 percent.
“We’ve been able to go in and help these growing organizations benchmark each of these acquired physician offices to show where they are at in terms of their safety protocols,” Osborne said. “It helps risk managers know where they need to start.”
Ambulatory Safety
Another major challenge for patient safety is the movement of care away from main hospitals to ambulatory care settings, an area that previously did not concern hospital-based risk managers very much.
“Historically, there has not been a big focus from a patient safety standpoint on outpatient services,” Osborne said. “The office practice assessment that AIG’s been doing for the last two or three years has actually put us out in front. Few other resources out there can assist hospital-based risk managers in dealing with outpatient-type services.”
“Now more people are thinking about safety in ambulatory areas, and we have more knowledge and experience there,” Killen added.
The same office assessment tools that survey physician practices can also be applied to ancillary services like ambulances, blood banks, and outpatient surgery centers, though benchmarking is not yet available for these sites.
Advancing Technology
 Adapting to new technology is an ongoing challenge for health care risk managers.
Adapting to new technology is an ongoing challenge for health care risk managers.
“Everyone thought electronic health records were going to solve all our patient safety issues, but they’ve come with some unintended and dangerous consequences,” Killen said. Employees may accidentally order medications for or even discharge the wrong patient, for example, if they have multiple records open at once.
The upside to technology advancements, though, is more streamlined documentation and more opportunities for communication between doctors and patients via telemedicine, which is slowly growing in popularity for remote and elderly patients.
“When we’re underwriting, we look at these areas of growth in technology and the many ways it can be applied,” Osborne said. “We consider all the pros and cons.”
Standout Services
Lexington’s dedication to improving safety in health care shines through in their thorough assessment tools, expert recommendations, and attention to insureds’ changing risk management needs.
“Our unique tools help insureds identify risks and minimize potential claims,” Killen said.
“These services are homegrown and developed by a lot of very knowledgeable people over a period of time,” Osborne said. “They’re not available out in the market, and only Lexington insureds have access to them.”
For more information about Lexington Insurance’s risk management services for the health care industry, please visit www.lexingtoninsurance.com.
This article was produced by the R&I Brand Studio, a unit of the advertising department of Risk & Insurance, in collaboration with Lexington Insurance. The editorial staff of Risk & Insurance had no role in its preparation.










