Medical Costs
Fee Schedules Do Their Job, Despite Expensive Care
Physician fee schedules exist to help to control costs, but they can also have the unintended consequence of incentivizing doctors to push prices as high as they can. The National Council on Compensation Insurance released a research brief in April, “The Price Impact of Physician Fee Schedules,” that highlighted the costliness of treatment provided under workers’ comp versus group health plans, perhaps driven by the very fee schedules meant to contain them.
Problems arise when the maximum rates allowed by fee schedules are high relative to prices charged for group health and Medicare, and when a significant proportion of workers comp payments approach that max rate.
“Whether due to negotiated arrangements between workers’ comp insurers and their provider networks or to doctors acting individually, this occurs so frequently to suggest that fee schedules in fact set the prices that many medical providers charge for workers’ comp services,” the study said. One consequence is that some providers may be “charging [workers’ comp] claimants more than they would patients covered under Group Health.”
The margins varied both by specialty and by state.
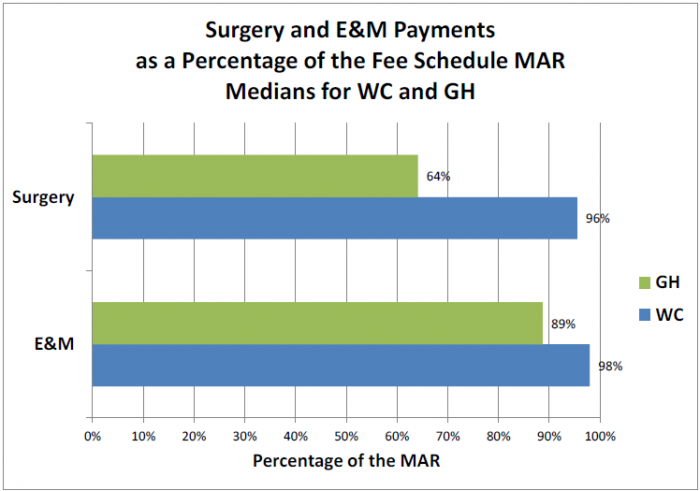
In surgery, for example, the median payments made for workers’ comp patients were at 96 percent of the maximum allowable rate (MAR). Median payments made for patients covered under group health plans, on the other hand, were at 64 percent of the MAR. For evaluation and management, however, the difference was not as large. Median payments for workers comp’ were high at 98 percent of the MAR, but median payments under group health were not far behind at 89 percent.
 “The main thing is that for surgery in general, fee schedules seem to be set higher relative to group health prices than for other specialties or general practice physicians,” said John Robertson, one of the study’s authors. “We don’t really know what individual physicians consider when they send a bill for work comp services, but we do see a large share of services billed right at the fee schedule.”
“The main thing is that for surgery in general, fee schedules seem to be set higher relative to group health prices than for other specialties or general practice physicians,” said John Robertson, one of the study’s authors. “We don’t really know what individual physicians consider when they send a bill for work comp services, but we do see a large share of services billed right at the fee schedule.”
Broken down by state, the study authors found that there was no uniform approach to setting fee schedules that established a set relationship between MARs, prices paid for workers’ comp and prices paid for group health. Discounts offered off the MAR were all over the map. Idaho offers five percent off the max rate, while Arizona, for example, offers 36 percent off. Nonetheless, payments made for group health were still only about 60 percent of prices paid for workers’ comp in both states.
This variation creates the impression that physician fee schedules are ineffective at keeping workers’ comp costs controlled and on a level playing field with the rest of the medical care marketplace, though the report suggests that the conclusion is not so simple.
“There certainly can be reasons why work comp prices should be higher than group health,” Robertson said, “There’s a different relationship between doctor and patient, and in some cases there’s more administration required.”
The Workers’ Compensation Research Institute also released a set of studies regarding differences in prices charges by ambulatory surgery centers (ASC) versus hospital outpatient settings in states with and without price regulation.
In states where fee schedules existed, services at ambulatory surgery centers were less expensive and charges were more predictable.
According to one study, “Payments to Ambulatory Surgery Centers”, “the average ASC payment for a common knee arthroscopy in the median state without a fee schedule ($6,272) was nearly double the median payment of the states with fixed-amount fee schedules ($3,174). Similar patterns were also found for shoulder surgeries.”
Richard Victor, executive director of WCRI, said, “We’ve also compared surgeons’ fees and office visits for an identical patient, paid by workers’ comp and also by group health insurers. For the surgeons, workers’ comp is often much, much higher. For primary care, it’s higher about a third of the time, lower a third of the time, and another third of the time they’re in the same neighborhood. The big differences will be for surgeons, radiologists, neurologists and specialists.”
Asked if states should adopt a standard approach to setting fee schedules to ensure more even pricing across the board, Victor said states’ unique medical marketplaces would make that solution impractical.
“Many states would either overpay, or many states’ workers would have problems with access to care,” he said. “If you look at commercial insurance prices, there is a noticeable difference from state to state, based upon competitive conditions. In Wisconsin, the reimbursement rates for group health are much higher than they are in Minnesota, or Illinois. That’s just because of different market structure.”










