Air Ambulance Used for Injured Workers Takes Insurer to Court Over Medical Bills
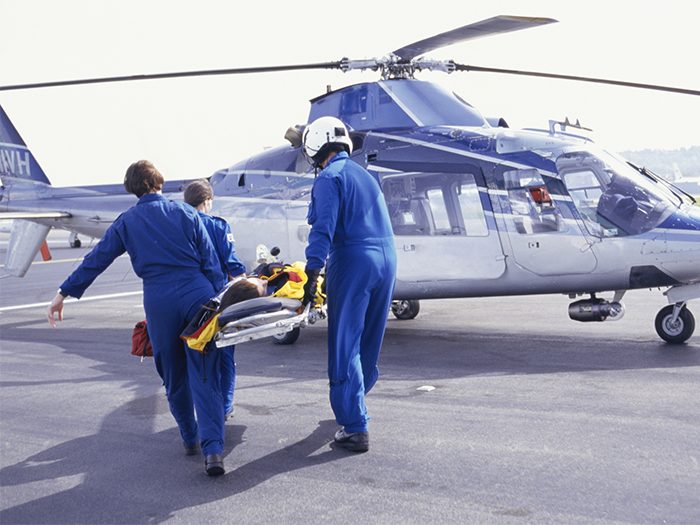
EagleMed, a privately owned and operated air medical transport service, was utilized by four separate employers to transport four separate injured workers.
EagleMed was used in all four instances to transport the workers from rural hospitals to larger ones that were better equipped to help them.
Workers’ compensation was administered to these employees through their work. Coincidentally, all four employers had workers’ comp insurance policies with Travelers Insurance. And, in all four instances of air ambulance transport, Travelers did not preapprove the flights.
EagleMed submitted invoices ranging from $21,000 to upwards of $33,000 for the services provided. Travelers said the invoices were unreasonable and offered reduced payments of $4,000 to $8,000 based on its interpretation of what would be paid under federal Medicare reimbursement rates.
EagleMed pursued legal action, filing a fee dispute with the Kansas Division of Workers’ Compensation, where the four individual claims were consolidated into one.
Travelers argued for reduced payments based on Medicare payment calculations, while EagleMed said that Travelers should be on the hook to pay the bills in full.
The hearing officer reserved judgment on what EagleMed could charge or what Travelers was responsible to pay.
Both parties appealed.
The Workers’ Compensation Appeals Board then reversed the hearing officer’s decision, and the hearing officer decided “the Division lacked authority to set any reasonable and necessary payment rates for air ambulance services through either the rate-setting regulatory process or an administrative appeal proceeding.”
EagleMed would be paid in full.
Again, Travelers appealed, but the Workers’ Compensation Appeals Board said it lacked the “jurisdiction to decide whether the Medicare fee schedule could be applied to air ambulance rates in workers’ compensation cases,” thus affirming the hearing officer’s ruling.
Travelers was not finished, however, and sought judicial review. In this review, Travelers argued the Workers’ Compensation Appeals Board erred by saying it did not have jurisdiction to decide. This error, Travelers posited, could be corrected by limiting EagleMed to an amount “mandated by federal law,” which could be the Medicare fee schedule.
EagleMed disagreed. It did agree that the Board erred by saying it lacked jurisdiction, but it further argued that Kansas law and the Airline Deregulation Act combine to entitle the air ambulance to its “full billed charges.”
“Eliminating air ambulances from the Kansas workers’ compensation system will have enormous negative consequences for workers and employers in this state,” EagleMed representatives said.
Scorecard: Upon review, the appeals court judge ruled that the Kansas Workers’ Compensation Appeals Board should have determined whether the charges issued by EagleMed were “usual and customary” for the services rendered before it ordered payment. The Board is left to decide.
Takeaway: When dealing with workers’ compensation claims, particularly the more complex ones, it is best to know what is covered under you policy prior to incident in order to guarantee both payment is there and your workers are receiving the proper care. &










