WC Cost Control
Air Ambulance Rate Debate Unlikely to Fly Away
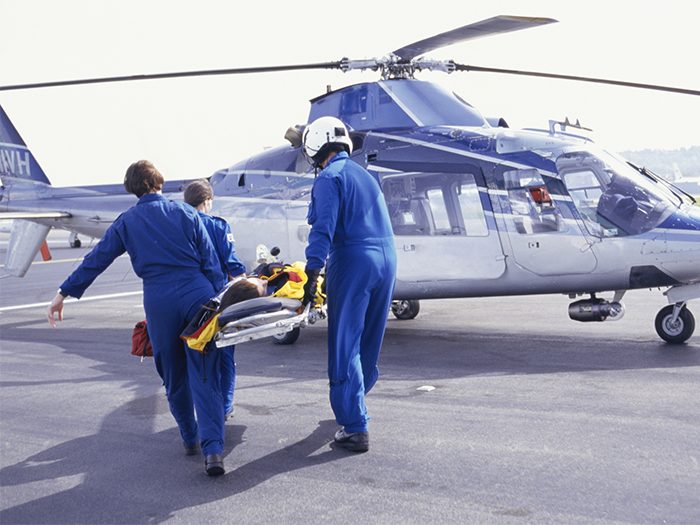
Disputes over air ambulance transport bills continue to rage on, and a recent ruling in Texas overturning a decision in favor of insurers isn’t likely to ground the debate.
More than a half a million individuals are transported via air ambulance services each year, according to the Association of Air Medical Services. The majority of these transports are via helicopter in emergency situations; the remainder are fixed-wing transports for longer distances.
While fees charged by traditional medical transport services are regulated under the Affordable Care Act, air ambulance providers argue that they fall under the jurisdiction of the Airline Deregulation Act (ADA) of 1978, which prevents states from enacting or enforcing laws or regulations related to the price, route or service of an air transportation carrier.
This, unfortunately, has led to runaway transport fees and no way for insurers to mitigate them.
Linda Colsen, vice president and national product leader at Jacksonville, Fla.-based One Call Care Management, said emergent care situations where an individual needs to be transported via helicopter to a trauma center is the biggest contributor to these runaway rates.
“The call is being made on the ground in an emergency situation by the local EMS provider, and from a payer perspective, there’s no oversight, no ability to negotiate savings, and they’re stuck with the invoice that can be tens, even hundreds of thousands of dollars,” she said.
Colsen said one of her clients was billed more than $300,000 for a single helicopter emergency transport, but that One Call was able to negotiate savings of $173,000 for the insurer during a retrospective review.
Excessive helicopter transport bills were the crux of the lawsuit in PHI Air Medical, LLC v. Texas Mutual Insurance Company, et al. A trial court rendered judgment in favor of eight plaintiff insurers, which included Texas Mutual Insurance Company and Hartford Underwriters Insurance Company, who disagreed with PHI’s per-trip charge for medically transporting injured workers.
On Jan. 31, 2018, however, the Texas Court of Appeals remanded the case, holding that any rate provisions for air ambulance transports are preempted by the ADA.
Under the Texas Workers’ Compensation Act, the state’s Commissioner of Workers’ Compensation has the right to adopt policies and guidelines that reflect standardized reimbursement structures by using Medicare and Medicaid reimbursement methodologies and policies, and to ensure that these guidelines are fair and reasonable “to ensure the quality of medical care and to achieve effective medical cost control.”
The Act also defines a maximum allowable reimbursement (MAR) for workers’ comp-related medical costs, setting this MAR at 125 percent of the Medicare or state Medicaid fee schedule, or a “fair and reasonable rate” if neither applies.
While the trial court held the insurers could not be asked to pay more than 125 percent of the Medicare amount for air ambulance transport, the appeals court said the ADA’s preemption provision bars a state from enacting a law or rule “related to a price, route or service of an air carrier that may provide air transportation …”
Interestingly, the court did not demand that the insurers pay the air ambulance company.
“From a payer perspective, there’s no oversight, no ability to negotiate savings, and they’re stuck with the invoice that can be tens, even hundreds of thousands of dollars.” — Linda Colsen, vice president and national product leader, One Call Care Management
Mary Nichols, senior vice president and general counsel for Texas Mutual, said these court decisions have left no pathway to payment, and noted that the courts have not identified a single provision in the ADA or other federal statutes that would require state actors to make any payment of air ambulance claims, “much less at the rates they choose to charge.”
Although multiple states have enacted laws to combat unfair air ambulance charges — leading to dozens of lawsuits — they’re ineffectual unless Congress decides to make a change to the ADA.
“They are subject to challenge unless the courts or Congress clarifies the issue,” Nichols said. “Until then, states may lack the authority to order payment of any kind, including billed charges.”
Sen. Jon Tester, D-Montana, introduced S.B. 471 in February 2017, which would create an exemption in the ADA to allow states to regulate air ambulances. Although the bill has the support of the National Association of Insurance Commissioners, it hasn’t left committee.
The courts could eventually clarify the issue too. Nichols said Texas Mutual will be filling a petition for review with the Texas Supreme Court, and noted that a similar case in West Virginia is on appeal to the 4th Circuit Court of Appeals.
The top executive of one southeastern air transport company said brokers who arrange services — some of whom may inflate the bill by as much as three to four times the actual cost of transport — are also a part of the problem. The executive, who asked not to be identified, said his company coordinates air ambulance services, and about 80 percent of its business involves coordinating services for workers’ comp clients.
He noted that he doesn’t see a reimbursement cap of 125 percent of Medicare as unreasonable. But he believes further attempts to implement legislation in the industry will receive significant push-back from brokers.
“There has to be a reasonableness that is fair to the broker and that is fair for the payer based upon the actual cost of rendering the services,” said the executive. &