Preparing for the Long-Haul: How Today’s COVID Claims Will Likely Impact Workers’ Comp for Years to Come
The COVID-19 pandemic is nearing the one-year mark in the United States, and as we learn more about the virus’s assault on the respiratory system, a new threat with potentially devastating effects on workers’ compensation payers has emerged.
Post-acute COVID-19 syndrome, an illness which can linger for months and is characterized by a myriad of difficult-to-diagnose symptoms, is now top of mind for claims organizations.
The CDC identified the condition and studied a cohort to determine what lingering effects the virus might have on sufferers who survived the ordeal and were discharged.
They found that 58% of patients reported new or worsening difficulty completing activities of daily living in a 60-day post-discharge phone survey.
Further, “among 195 patients who were employed before hospitalization, 117 had returned to work while 78 could not because of ongoing health issues or job loss. Of the 117 patients who returned to work, 30 reported reduced hours or modified duties due to health reasons.”

Michele Tucker, vice president of enterprise comp operations, CorVel
According to Karen Thomas, director of case management innovation at CorVel, the symptoms are indeed limiting for the individuals that develop them.
“We have encountered some claims where we have seen folks affected by post-acute, otherwise known as long-haulers. Some of the most common signs that we’re seeing that linger over time are fatigue, shortness of breath, cough, joint pain, chest pain and brain fog,” Thomas continued.
“There are also other symptoms we’ve seen as part of this syndrome, including muscle pain, headache, heart palpitations, loss of smell and taste long term, concentration and sleep issues, and even hair loss. We’re having folks report all of that, and depression,” she said.
Long-term COVID Delays Return-to-Work
Further complicating these post-acute symptoms is their effect on return-to-work, which can be stalled or delayed.
Michele Tucker, vice president of enterprise comp operations, also with CorVel, noted that she has encountered patients facing the “inability to complete their work because of fatigue and because of concentration issues,” adding that it worsens because “we don’t see a lot of folks go back in a modified capacity, but what I am seeing in those lingering cases is that they’re being taken back off work.”
In these lingering cases, especially those that involved a hospitalization and the extended use of a ventilator, COVID files are beginning to be perceived the same way as a typical injury claim with cascading effects.
“The respiratory muscle weakness [caused by ventilators] is not something that’s going to resolve quickly and it will possibly impact them for a long period of time,” said Zack Craft, vice president of durable medical equipment and CarePath for OneCall.
“The way we see COVID claims is that the virus itself is more a mechanism of injury for these individuals; it’s no different than somebody falling off a ladder and the clinical impact is a spinal fracture and then they also have kidney issues. These COVID secondary issues are all over the board.”
COVID-19 Tests the Biopsychosocial Model
Secondary issues are also veering into the mental health space, testing carriers’ ability to actually provide the oft-touted biopsychosocial approach to the care of injured workers.
“The psychosocial is a huge part of it,” said Lisa Haug, managing director of the medical management unit at Safety National.
“They’ve been in that hospital, sometimes for months, sometimes on a ventilator, which greatly impacts their recovery. As a result of COVID-19, patients experience
a significant amount of brain fog whether on a ventilator or not. In addition to the brain fog, it’s the psychosocial components — not being with loved ones, not having the family support because no one is allowed to visit.”
With brain fog on the low end of the spectrum, reported COVID-19 mental health effects can extend to post-traumatic stress-adjacency.
“We have been seeing what’s called post-COVID-19 traumatic stress syndrome (PCTSS) and there’s a lot of anecdotal information on this, and this can happen even in mild cases,” Thomas said.
“In the more severe cases, it has to do with the symptoms an individual is experiencing and with going back to work. There are components of depression and anxiety that we’re seeing across the board, even for folks who have not had COVID-19.”
In response, CorVel trained 80 nurses who have gone through a certification process to assist with PCTSS.
The need for such interventions is especially profound for claimants working in the health care field, who may develop PCTSS as they prepare to return to work.
Calling the pandemic “a bio-disaster with profound psychological effects on health workers,” a June 2020 study of nurses exposed to COVID in China found that the rate of PTSD symptomology reached 16.8%, most of it associated with avoidance behavior.
Should similar rates manifest in the United States, the effect on workers’ comp exposure across jurisdictions could be significant, but according to some, expected.
“The psychophysiological and psychosocial effect on the resolution of workers’ compensation injuries is most certainly not new,” said Carol Ungaretti, managing consultant at Aon.
“What’s new, in my opinion, is the fact that many of us in the insurance industry are actively designing and implementing a strategy to identify mental health issues early in the life of a workers’ compensation file,” said Ungaretti.
We believe mental health issues will most certainly impact COVID-19 claim outcomes and that it is imperative early interventions are appropriately deployed to ease the negative effects associated with disruption of full duty return to work, including addressing employee fears of contracting COVID or another similar disease,” Ungaretti continued.
Jurisdictional Struggles Abound
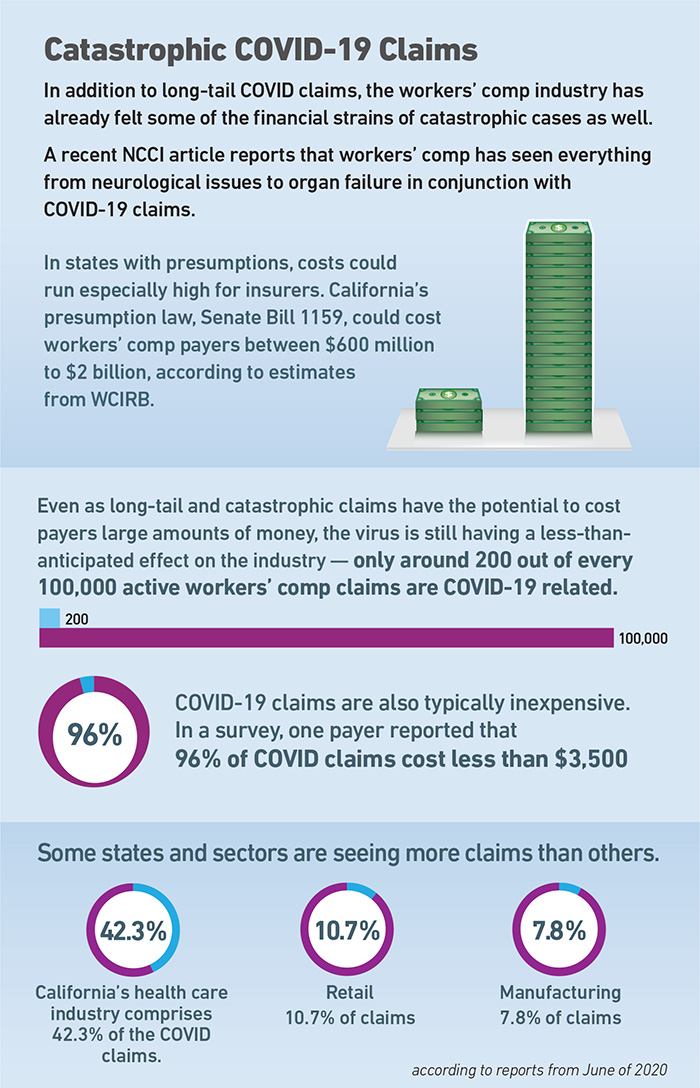
In addition to mental health strategies to provide the best outcomes for patients, workers’ comp carriers are still facing the windfall of jurisdictional changes associated with the pandemic, including presumptions.

Zack Craft, vice president of durable medical equipment and CarePath, OneCall
Brent Bland, senior vice president and head of workers’ compensation claims at AmTrust, noted that his organization’s strategy for managing COVID claims has remained the same since the beginning.
“From a strategy and loss handling standpoint, we’ve stayed very consistent with how we have approached this event. We have greater clarity around statutes, presumption laws, medical care and impact,” he said.
AmTrust trained claims handlers on investigative guidelines, as well as statutory provisions. “If there are situations where there are reduced hours, each state is different and we’ll have to assess each case based on the individual facts and the state laws and presumption orders,” Bland explained.
“A key consideration is whether the reduction in hours is because of an accepted claim or some reason unrelated to the injury or illness. There’s the possibility that someone could be eligible for indemnity benefits or permanency — all jurisdictionally driven.”
With the available data surrounding COVID-19’s acute and chronic effects standing at only about a year old, the race to analyze outcomes on the organizational level is paramount and can act as a balm for the virus’ uncertain impacts.
“It’s a scary time for payers, because these claims have the potential to become the next mega claims, which can be devastating to payers and employers,” said Linda Colsen, OneCall’s vice president of customer experience.
The singular likely reprieve from new COVID claims and the additional long haulers they bring is widespread vaccination, which has faced manufacturing and distribution delays on both the state and federal level since the initial two versions were approved in 2020. Until then, concerns abound. &










