Sponsored Content by Concentra
Chasing Pain Complaints Doesn’t Work: Why Function Belongs at the Center of Workers’ Compensation Care

Body temperature, pulse, respiration and blood pressure. These are the four primary vital signs used by doctors and nurses to measure your body’s most basic functions and detect life-threatening medical problems. Or at least they were until 2001, when the Joint Commission dubbed pain “the fifth vital sign.” The designation was the result of a years-long push by some medical professionals and the pharmaceutical industry to do more about patients’ pain.
“There was a growing narrative that we perhaps shouldn’t allow people to suffer unnecessarily when wonderful medications were available to treat pain,” said Dr. Maja Jurisic, Vice President, Medical Director of Strategic Accounts, Concentra Occupational Health. “It became standard of care to ask patients to rate their pain on a scale of 0 to 10.”
Pain as a metric for recovery permeated the healthcare industry at large and had an outsized impact on the way workers’ compensation claims were managed. For many clinicians, recovery wasn’t considered complete until pain resolved, so claims could stay open as long as pain persisted.
This had multiple negative consequences for payers, employers and most importantly, injured employees.
“We need to shift the focus away from pain and toward function and overall wellness,” Dr. Jurisic said. “Doing so can support a speedy recovery and get injured employees back to their jobs and normal lives faster.”
Why Treating Pain Doesn’t Work

Dr. Maja Jurisic, Vice President, Medical Director of Strategic Accounts, Concentra Occupational Health
The practice of rating pain at every medical appointment has created the misconception that pain is inherently linked with the status of recovery from an injury. But it’s understood now that the experience of pain can be separate from the strains, sprains, breaks and tears that constitute the injury itself.
The International Association for the Study of Pain defines pain as “an unpleasant sensory and emotional experience associated with actual or potential tissue damage.”
“Pain may or may not be correlated with injury severity or the state of healing,” Dr. Jurisic said. “The very same neural pathways that are activated by physical pain are also activated by emotional pain. And a lot of people don’t differentiate.”
An injured employee may believe that if his back hurts more today, he must not be getting any better. But if he just had an argument with his wife, or is worried about the family’s finances, or is feeling frustrated being out of work — all those emotional stresses can feed the perception of pain.
“Unless physicians take that into account when dealing with injured employees, we’re going to go down a lot of dead ends and take a lot of detours. And that’s exactly what happens,” Dr. Jurisic said. “There are many unnecessary diagnostic tests and procedures done when physicians chase pain complaints without considering whether it even makes sense medically. And it’s no coincidence that the rise of opioid addiction coincided with the increased focused on pain management.”
Medicalizing emotional pain, and assuming all pain complaints correlate with “tissue damage,” even when that is not supported by exam and/or other diagnostic findings may slow down recovery by creating a mindset of fear. Thinking that something dangerous is going on in their bodies increases anxiety and feeds their perception of pain. Neural pathways are trainable; they grow and change in response to stimuli. The more injured employees are asked about pain, the more they think about it. The more they think about it, the better their neural pathways get at producing pain. After a time, they “learn” pain, which can persist long after their tissues have healed.
Constantly focusing on pain can cause an individual to feel broken and limited in their physical capabilities, which can be the beginning of a path toward psychological problems like depression and reliance on painkillers.
As claims drag on without any improvement in pain, medical providers and employers may become skeptical of the injured employee’s complaints.
“They’re not necessarily exaggerating. They are feeling real pain, even though it’s out of proportion to objective findings. And if they begin to feel that no one is helping them, an angry victim mentality, in my experience, becomes a big barrier to a successful return to work,” Dr. Jurisic said.
Bringing the Focus Back to Function and Wellness
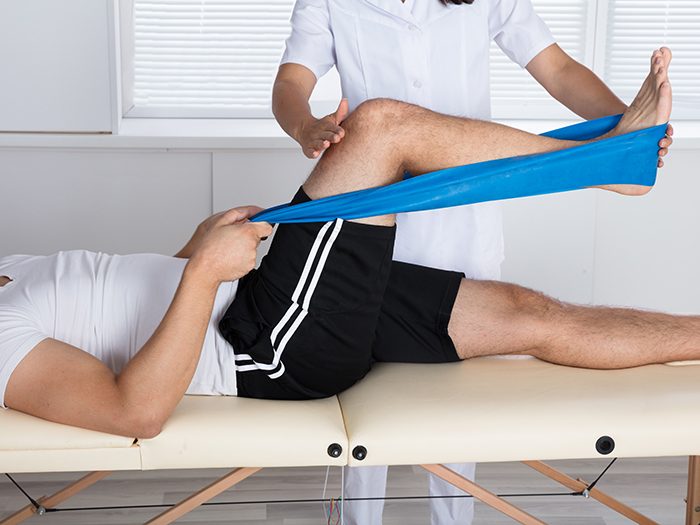 A better way to measure progress is to assess objective findings, and what an injured employee can do.
A better way to measure progress is to assess objective findings, and what an injured employee can do.
For an employee with a sprained ankle, for example, recovery might be measured by his or her ability to fully flex and extend the joint, place their full weight on that foot, and walk with a normal gait.
Function-based assessments more accurately reflect what state of healing the damaged tissue is in and filter out subjective ratings of pain. This keeps medical practitioners from going down the potential rabbit hole of “curing” pain, and it stays true to the purpose of workers’ compensation care — restoring the capabilities that injured employees need to perform their jobs.
Focusing on function also turns a negative experience into a positive one. Thoughts turn away from pain and toward performance.
“How you think about yourself and your capacity makes a big difference in what you’re able to do,” Dr. Jurisic said. “If you think of yourself as disabled, you’re not going to get better very quickly. If you think of yourself as a person who still has abilities and can still contribute, you have a greater sense of value and self-worth.”
Psychological resilience is just one factor in a holistic approach to treatment. In workers’ compensation, it’s common to focus on the compensable injury in isolation, but whole-body wellness is critical to efficient healing. That includes good nutrition and sleep hygiene as well.
“Restorative sleep goes a long way in helping tissues heal,” Dr. Jurisic said.
Shifting the Paradigm of Care in Workers’ Compensation
The challenge in eschewing the prioritization of pain lies in getting clinicians to go against their training.
“Most people trained in Western medicine take a mechanistic approach to care because that’s what they’re trained to do. You identify the pain generator, and you fix it,” Dr. Jurisic said. “So, we are constantly re-educating clinicians and trying to open their minds up to different approaches that have emerged since their training.”
A Concentra, the education effort involves sending daily clinical messages to physicians and therapists, reminding them to think of injured employees as whole people and consider all factors that could be influencing their recovery.
“How can you focus your conversation to help this person move forward if they have a dysfunctional way of thinking about their situation?” Dr. Jurisic said.
Concentra also got rid of the pain scale altogether (after the initial injury visit).
“We don’t use that anymore at rechecks. We replaced it with a functional restoration/status of healing scale based on job requirements,” Dr. Jurisic said. “We call it the FReSH scale. If an employee’s job requires lifting 50 pounds, that will be our goal, and we gauge their progress towards that goal. Concentra therapists have a template where they fill in objective data around what the injured employee is able to lift, push, pull, carry, etc.”
There’s also a system in place to catch outliers. A data analytics team flags cases that have unusually long case duration, more than the average number of PT visits, referrals to specialists, or lack of continuity of care. These cases – which constitute a small percentage of Concentra’s claims – get reviewed again by Center Medical and Therapy Directors, and then by more senior clinical leadership. Taking a step back to see the arc of a case provides an opportunity for mentoring and allows clinicians to alter their approach and try alternative strategies to help injured employees who are stuck move towards functional restoration.
“These are the cases that end up costing everyone the most money. Since we implemented this review process, we’ve decreased the duration of those outlier cases by about a month,” Dr. Jurisic said.
“What we’ve seen is that many people get better no matter what. Our bodies are beautifully designed to be self-repairing. But we have an opportunity to improve the process of return to work for even the most vulnerable people, those who have little resilience near the end of their coping skills, without the additional risks introduced by chasing and treating pain complaints that are not supported by objective findings.”
To learn more about Concentra, visit https://www.concentra.com/.
This article was produced by the R&I Brand Studio, a unit of the advertising department of Risk & Insurance, in collaboration with Concentra. The editorial staff of Risk & Insurance had no role in its preparation.